You wake up one morning covered in red, swollen welts that burn, itch and sting. Hives! Those mysterious, frustrating, incredibly irritating bumps that seem to appear out of nowhere. Take a deep breath – this article will cover what causes hives, as well as provide some practical tips to ease your discomfort.
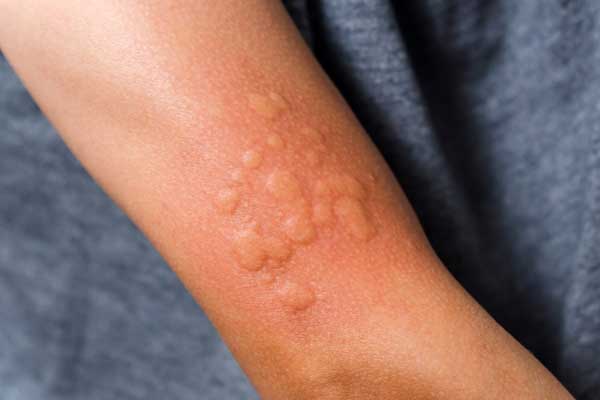
What Are Hives?
Hives, also known as urticaria, are a kind of rash characterized by sudden outbreaks of raised, flat-topped bumps and welts on the surface of the skin. Ranging in size from a few millimeters to the size of a dinner plate, hives tend to be red or skin-toned in appearance. The welts themselves are often surrounded by flushed, reddish skin.
In addition to their distinctive appearance, hives are almost always incredibly itchy or irritating. The welts themselves tend to burn, sting and itch, sometimes intensely. The surrounding skin may also itch, sting or feel like it’s burning.
Hives are not contagious. They’re caused by the person’s own histamine response, not an external pathogen or infection.
What Causes Hives?
Hives are caused by the release of histamine and other inflammatory factors in the skin. Histamine is released by immune system cells in response to an external trigger. The end result is fluid leaking out of tiny blood vessels into the surrounding skin, causing the swollen, itchy welts.
The tricky thing about hives is that the trigger is often unknown. In around half of all cases of hives, no cause is ever identified. However, some common triggers and contributing factors for hives include:
- Insect stings
- Pet dander
- Certain foods
- Medications
- Latex
- Heat or cold temperatures
- Stress and anxiety
- Infections
- Physical irritants (e.g. water, pressure on the skin)
- Exercise
People with asthma or hay fever allergies tend to be more prone to developing hives as well.
In most cases, a trigger causes a temporary hives outbreak lasting a few hours to a few days. The welts and irritation tend to fade on their own over time. However, new welts may continue appearing every few days or weeks if the person can’t identify and avoid their trigger.
Treating and Managing Hives
While frustrating, hives are typically harmless and tend to fade without treatment within 6 weeks. However, treating hives can help provide symptom relief. Here are some tips:
Cool Compresses
Placing cool, wet washcloths or compresses on hives can help ease burning and itching. The cool temperature helps constrict blood vessels and reduce inflammation. Don’t place ice directly on the skin, however, as this could damage skin tissue.
Lukewarm Showers
Taking lukewarm (not hot!) showers or baths can also soothe irritated skin prone to hives outbreaks. Avoid long soaks over 10 minutes, and use gentle, fragrance-free wash products to prevent further irritation.
Pat Dry and Moisturize
After bathing, gently pat the skin dry using a soft towel. Rubbing or scrubbing the skin can worsen irritation. Apply a gentle, fragrance-free moisturizer while skin is still slightly damp to help nourish, hydrate and calm the skin.
Cotton Clothing
Wear loose, lightweight cotton clothing to avoid trapping heat and sweat against the skin. Tight elastic bands around wrists, waist or other areas prone to hives should be avoided.
Anti-Itch Creams
Over-the-counter anti-itch creams containing pramoxine or menthol can provide cooling relief from hives-related itching. These numb and cool the skin upon application.
Antihistamines
For moderate or severe hives cases, oral H1 antihistamines help counteract the effects of histamine in the body. First-generation OTC options include diphenhydramine (Benadryl) and chlorpheniramine (Chlor-Trimeton). Newer prescription antihistamines like fexofenadine (Allegra) or cetirizine (Zyrtec) cause less drowsiness.
Corticosteroids
For severe hives unresponsive to antihistamines, oral corticosteroid medication like prednisone may be prescribed. These drugs work by broadly suppressing the immune system and inflammation. Use is generally short-term only, due to side effects.
Identify and Avoid Triggers
If hives continue recurring, keep a detailed log of foods eaten, activities, weather conditions and other factors in the hours leading up to an outbreak. This can help identify the trigger, allowing you to avoid it.
See an Allergist
For moderate to severe recurrent hives with an unknown trigger, see an allergist. Allergy testing can help identify potential triggers, and provide guidance on avoiding exposures.
The Bottom Line
Hives arise suddenly and mysteriously in response to histamine release in the skin. Causing red, swollen, itchy and irritating welts, hives tend to fade away again after a few hours or days. While frustrating, the itching and discomfort associated with hives can often be managed at home using some simple techniques. However, recurrent or severe hives may require prescription medication and medical investigation to identify underlying triggers.
